Yes, intermittent fasting probably does increase the risk of death from cardiovascular disease
A contrarian take on a recent deeply flawed study, whose conclusions are nonetheless almost certainly correct

A new study purports to show a 91% in cardiovascular disease death risk among those who intermittently fast, with a feeding window of 8 hours or less per day. Health writers competed to debunk and denounce the study in the strongest terms. Among some of the legitimate criticisms, we can include:
The “study” is just a poster and abstract presented at an American Heart Association conference, and the full paper has not yet been peer reviewed or published;
The data are self-reported from NHANES, which can be notoriously inaccurate across certain dimensions of diet, the most well-known of which is energy intake. Those who “reported” eating within an 8-hour window might not have actually done so;
There was no adjustment for relevant confounders, so we cannot know if the people who eat fewer than 8 hours per day might not simply be at higher risk of cardiovascular disease in the first place;
To build on 3, observational studies have residual confounders which are impossible to control for, making their findings inherently weaker than randomized controlled trials.
I agree with these criticisms.
The study really is flawed, and we cannot draw strong causal inferences from it.
But, the study’s conclusions should still be taken seriously: they are probably right. And that is because what the rest of the scientific literature broadly agrees with the study’s findings.
But this is not for the reasons one might think. The problem isn’t the small window. The problem is with the way a smaller window is (nearly always) implemented. Thus, it is probably true that, in the real world, consuming food within a small feeding window is deleterious to cardiovascular health. But not because the window is small.
We should start by discussing the vast amount of research conducted over the past half-century showing that mammalian metabolism is highly regulated by the day-night cycle. Meals consumed earlier in the day produce lower glucose and triglyceride levels in the blood. And meals consuming later produce higher levels.
We can see this in the following figure:
What this shows is that late-day eating produces larger glucose spikes. Since these glucose spikes are associated with cardiovascular disease risk, probably causally, this means that late-day eating, all else equal, probably results in more cardiovascular disease risk.
But glucose is not the only cardiovascular risk factor that increases with late-day feeding. Blood pressure and LDL cholesterol, two other important cardiovascular risk factors, also worsen.
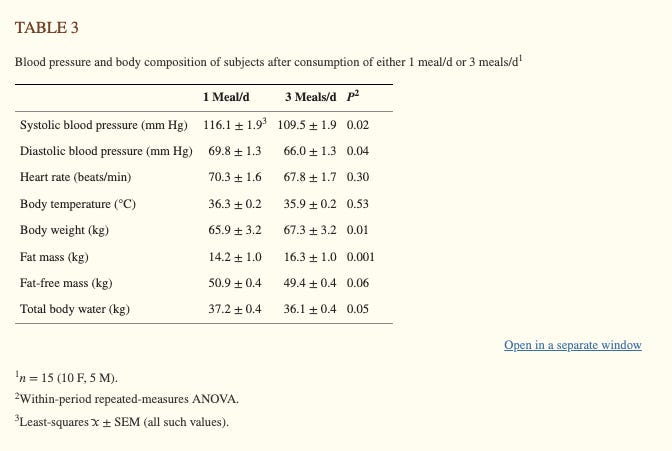
In this 2007 study, participants spent 8 weeks eating 3 meals per day, then 8 weeks eating 1 meal per day, in a crossover fashion. This means that each participant served as their own control. All evening meals were fed to participants at the research center. If participating in the one-meal-per-day phase, participants consumed the entire meal at the research center over the course of 4 hours, which consisted of a combination of all 3 meals that they would consume during the three-meal-per-day phase.
The researchers found that the participants lost slightly more weight during the 1-meal-per-day phase, likely because they “cheated less” when they went home.
Despite the lower body weight, their systolic blood pressure and diastolic blood pressure both increased.
Cholesterol and LDL cholesterol also increased.
Thus, even though participants lost weight, their cardiovascular disease markers worsened. This is remarkable, because the benefits of a loss of body weight usually overwhelm all other variables. Take the case of Professor Mark Haub, a professor who consumed what he called the “Twinkie Diet” at a calorie deficit, dramatically improving his cardiovascular risk markers. Even in Dr. Haub’s case, who lost weight consuming almost entirely junk food, the weight loss produced powerful health benefits, despite the deterioration of diet quality.
What this means is that the bodies of participants really did not like the one-meal-per-day regimen. The body is well-designed to utilize energy earlier in the day and poorly designed to do it in the evening.
Other studies tell the same story. Check out this one from 2021. It found metabolic deterioration from the kind of late-day fasting often advocated by intermittent fasting promoters. Meanwhile, the opposite form of fasting, which focused on eating most calories earlier in the day, was found to be associated with metabolic improvements.
Yet other study types show something similar. Well-controlled metabolic ward studies, providing a test meal earlier vs. later in the day, showed an acute deterioration in metabolic function for the meal given later in the day:
Here’s where we get to <8-hour-per-day eating schedules. Most people who restrict their feeding window do so to the evening. They do not eat a huge breakfast, then forgo all food until the next morning. They eat large dinners, then skip breakfast.
The problem with a smaller eating window is not the size of the window: it is the timing of the meal. A smaller window is probably good because, if the food choices are sound, a small window will usually produce a lower calorie intake.
But the timing of the meal has very important health consequences, regardless of the calorie intake or body weight. Given that intermittent fasting is not a very robust weight loss intervention at the population level (although it can work unusually well for some), great caution should be exercised about using it in the form of delayed/evening feeding.
It would be optimal, as Matthew Herper writes, to focus on the use of randomized controlled trials rather than observational studies, due to the weaknesses inherent in the latter type of study design. However, the downside of randomized controlled trials in nutrition is that we may never have them. It is necessary to piece together the science the best we can to come up with actionable plans, given what we have.
What we can conclude here is the commenters on this latest study are missing the forest for the trees. Although the study that is currently trending uses weak methods, these weak methods nonetheless, albeit perhaps for the wrong reasons, came to the right conclusion.






"Breakfast like a King, lunch like a Prince and dine like a pauper"?
Very interesting. Timing matters. Given that most people find it harder to avoid eating at night time, it seems curious that our bodies are more capable of handling food earlier in day versus evening.